16
JCN supplement
2015,Vol 29, No 5
CASE REPORTS
Slow-to-heal leg ulcer
Pat McCluskey, clinical nurse specialist in wound care,
Cork University Hospital Group
BACKGROUND
Mrs P was a mother of three in her mid-
forties. She led an active lifestyle until
recently when she developed a leg ulcer
on the anterior aspect of her left lower
leg following mole removal by her GP.
MEDICAL HISTORY
She had deep venous thrombosis in her
left (x2) and right (x1) legs, for which
she was treated with anticoagulant
therapy (warfarin). She had a
cholecystectomy at 40 years of age.
She smoked 10 cigarettes daily for 20
years but had stopped four years ago.
Since then she had gained considerable
weight (21lbs). Mrs P developed an
ulcer on her left leg three years ago,
which had healed with compression
therapy in 10 weeks. She continued to
wear compression hosiery for a short
period of time, but then stopped.
Bilateral leg ulceration
Lorraine Grothier, consultant nurse, tissue viability,
TissueViability Centre, Provide CIC
This lady had a history of long-
standing leg ulceration. Healing had
been achieved but on an episodic
basis and re-ulceration had
always occurred.
Initial examination revealed
X
X
an extensive area of ulceration to
the left medial gaiter area, and the
ulcer had been increasing in size
despite treatment with compression
bandaging. The majority of the
wound bed was covered in a layer of
slough, with no evidence of epithelial
advancement.
Despite treating with appropriate
wound management products and
compression bandaging, there had
been no significant advancement
towards healing for some time.
PICO
™
INTERVENTION
PICO
™
was used in conjunction with
a PROFORE
™
4-layer bandaging
system for three weeks, with
polyhexamethylene biguanide (PHMB)
gauze to lightly pack the shallow cavity.
During the 21 days of treatment
with PICO, the wound made significant
progress towards healing. The
condition of the wound bed improved
considerably, with islands of epithelial
tissue emerging within the wound.
Case report 2
Case report 1
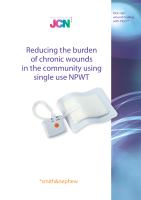
Figure 2.
Appearance of the wound before treatment
with PICO (left) and after 21 days of
treatment with PICO in conjunction with
multilayer compression bandaging (right).
Figure 1.
Application of PICO
™
and PROFORE
™
.
a
e
b
f
c
g
d
RECURRENCE OF LEG ULCERATION
After Mrs P’s GP removed a suspicious
mole from her left lower leg, the
resultant incision dehisced after the
sutures were removed revealing a
wound of 2.5x2.5cm.
Routine vascular investigations
revealed:
`
Anke brachial pressure index
(ABPI) = 1.1
`
Obvious haemosiderin staining
`
Ankle flare and oedema.
PREVIOUS MANAGEMENT:
YEAR ONE
Despite treatment for one year with
the‘Gold Standard’of graduated
compression therapy, there was no
progress towards healing.
In conjunction with compression
therapy, a variety of antimicrobial
dressings were employed to address
problematic bacterial burden. Oral
antibiotics were also prescribed on two
occasions to treat wound infection.
Mrs P was upset and anxious due to
the wounds’s failure to heal, despite a
year of intensive treatment.
Given the static nature of the wound,
a punch biopsy was taken which showed
stasis dermatis.
SURGICAL INTERVENTION
Mrs P was referred to the plastic
surgeon to be assessed for potential skin
grafting, and was admitted for surgical
debridement.
Extensive surgical debridement
of the wound and surrounding
inflammatory tissue and haemosiderin
staining was performed.
A split-thickness skin graft was taken
and applied to the wound in conjunction
with cannister-based negative
pressure wound therapy (NWPT) and
compression therapy.
At review five days later, there was
100% take of the graft — compression
therapy was continued and Mrs P was
discharged after a 10-week inpatient stay.
GRAFT FAILURE
At the initial outpatient clinic follow-up
appointment there was 50% loss of
the graft.
Bacterial burden was believed to